Water Blisters and Vesicles on Hands and Feet: A Complete Guide to Dyshidrotic Eczema
Are you troubled by small, fluid-filled blisters on your fingers, palms, or soles of your feet? It could be dyshidrotic eczema (pompholyx) – a chronic inflammatory skin condition that affects women twice as often as men and ranks among the most common dermatological consultations. In this article, you will find everything you need to know: from causes and symptoms to effective care.
TABLE OF CONTENTS
1. What is dyshidrotic eczema?
2. Symptoms of dyshidrotic dermatitis
3. What causes dyshidrotic eczema?
4. Risk factors and triggers
5. How is dyshidrotic eczema diagnosed?
6. Treatment of dyshidrotic eczema
7. Proper skin care for dyshidrotic dermatitis
8. Prevention and practical tips
9. Scientific references
What is dyshidrotic eczema?
Dyshidrotic eczema (medically known as pompholyx, also called dyshidrosis) is a chronic, relapsing form of vesicular eczema that is confined to the fingers, palms, and soles of the feet. It manifests as deep-seated, small blisters filled with clear fluid that itch intensely and can be painful (Lofgren & Warshaw, 2015).
The name "dyshidrosis" is historically misleading – although it has been associated with excessive sweating, histological examination confirms that the sweat glands are not directly affected. It is an eczematous reaction in the skin, not a disorder of sweating per se (Wollina, 2010).
The condition tends to recur in cycles – it typically worsens in spring and summer, during periods of increased sweating and more intense contact with allergens.
Symptoms of dyshidrotic dermatitis
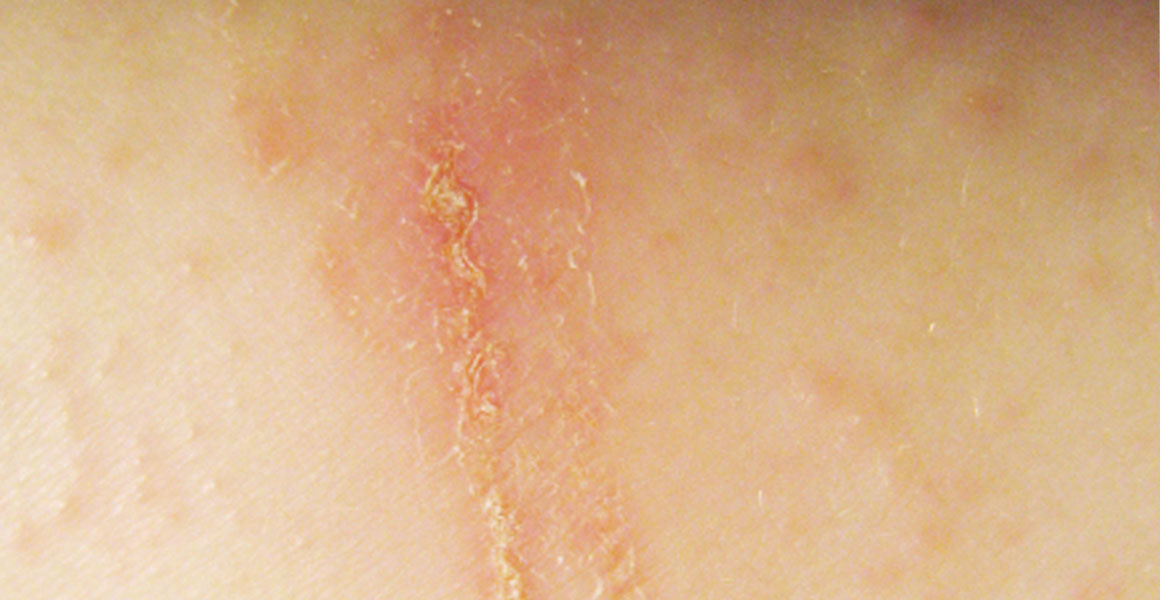
Dyshidrotic eczema has a typical course that differs from other forms of eczema:
PHASE 1 Initial phase
Small, "sago-like" vesicles (1–2 mm) filled with clear fluid appear on the sides of the fingers, palms, and soles. These blisters are deep-seated beneath the thick skin and itch or burn intensely.
PHASE 2 Advanced phase
Blisters may coalesce and form larger bullae. The surrounding skin becomes red and swollen. Intense itching leads to scratching, which increases the risk of secondary bacterial infection.
PHASE 3 Chronic phase
Blisters gradually dry out, the skin cracks, peels, and painful fissures develop. In long-term cases, the nails may also be affected – their colour, surface, and thickness change, with pitting and discolouration appearing.
When to see a doctor: If the blisters contain cloudy (purulent) fluid, the surrounding area becomes significantly red and swollen, or fever persists – these symptoms may indicate a bacterial superinfection and require professional treatment.
What causes dyshidrotic eczema?
The exact cause of dyshidrotic eczema is still not fully understood, although numerous theories exist. The scientific literature places it within the eczema spectrum and indicates that its development involves a combination of genetic, immunological, and environmental factors (Abreu-Velez et al., 2009).
The most commonly cited causes and mechanisms include:
Contact allergy to metals: One of the best-documented triggers is allergy to nickel, cobalt, and chromium. Contact allergy has been documented in approximately 30% of patients with dyshidrotic eczema. Interestingly, not only skin contact with these metals but also their ingestion through food can trigger flare-ups (Yoshihisa & Shimizu, 2012).
Immune dysregulation: Immunohistochemical studies have demonstrated the presence of T-lymphocytes (CD3, CD8), IgE antibodies, and complement components in affected skin, suggesting a complex immunological process involving both cellular and antibody-mediated responses (Abreu-Velez et al., 2009).
Skin water balance disruption: Recent research highlights the role of aquaporins (AQP3 and AQP10) – protein channels in the skin responsible for water transport. Their overexpression in the epidermis may contribute to skin dehydration and disease chronicity (Soler et al., 2015).
Other triggers: emotional stress, excessive sweating (hyperhidrosis), contact with irritants (cleaning products, solvents, soaps), climate changes, UV radiation, dermatophyte infections, and certain foods.
Risk factors and triggers
Based on published clinical data, the main risk factors can be identified:
|
ATOPIC PREDISPOSITION Up to 50% of patients have a personal or family history of atopy (eczema, asthma, hay fever). IgE levels are often elevated even in patients without known atopic diathesis (Medscape, 2024). |
FEMALE SEX Women have approximately a 4-fold higher risk of contact allergy to nickel compared to men, which explains the higher prevalence in females (Ahlström et al., 2019). |
|
|
OCCUPATIONAL EXPOSURE Higher risk is seen in hairdressers, bricklayers, healthcare workers, mechanics, and cleaning staff – professions with frequent contact with irritants or metals. |
STRESS AND SEASONAL INFLUENCE Psychological stress is a documented aggravating factor. Flare-ups occur most frequently in spring and summer, when temperature, humidity, and sweating intensity increase. |
|
How is dyshidrotic eczema diagnosed?
The diagnosis of dyshidrotic eczema is primarily clinical – an experienced dermatologist makes it based on the typical appearance and location of the blisters. In unclear or treatment-resistant cases, the following are performed:
Skin biopsy: Histology typically reveals spongiosis (intercellular oedema), intraepidermal vesiculation, hyperkeratosis, and a perivascular lymphocytic infiltrate (PMC, 2023).
Epicutaneous tests (patch tests): Used to detect contact allergy to metals (nickel, cobalt, chromium) or other allergens. In some patients, an oral metal provocation test may also be appropriate.
Mycological examination: To rule out dermatophyte infection, which can mimic dyshidrotic eczema.
Treatment of dyshidrotic eczema
Treatment of dyshidrotic eczema is often challenging and requires patience. Most patients need a combination of several approaches (Wollina, 2010):
1 Basic measures: Identification and elimination of triggers (allergens, irritants). Pay attention to what you touch, what you wash with, what you use for laundry, and what materials you wear.
2 Topical treatment: The foundation is potent topical corticosteroids during acute phases. Calcineurin inhibitors (tacrolimus, pimecrolimus) are an alternative. Aluminium acetate compresses help with weeping blisters – they "dry out" the vesicles and prevent secondary infection.
3 Phototherapy: PUVA (psoralen + UVA) and narrowband UVB phototherapy have demonstrated efficacy in chronic forms.
4 Systemic treatment: In severe, treatment-resistant cases, immunosuppressants (ciclosporin, methotrexate, mycophenolate mofetil), alitretinoin, or newer biologics (dupilumab, tralokinumab) may be considered.
5 Dermocosmetics: An essential part of care is suitable dermocosmetics that maintain hydration, restore the skin barrier, and soothe inflammatory processes. More in the following section.
Important note: Even with the right treatment, a short-term worsening may occur at the beginning as the skin's pH normalises and its natural biochemical processes are restored. This is normal and should not lead to premature discontinuation of care.
Proper skin care for dyshidrotic dermatitis
The key to long-term control of dyshidrotic eczema is consistent and regular skin care with suitable dermocosmetics that meet the following requirements: specifically designed for eczema-prone skin, containing anti-inflammatory ingredients, providing intensive hydration and restoring the disrupted skin barrier, and free from irritating fragrances and allergenic preservatives.
These criteria are met by EPIDERMA® dermocosmetics, which contain the patented anti-inflammatory composition Betuldiol®.
EPIDERMA® offers specialised comprehensive programmes designed specifically for eczematous skin. These programmes help soothe inflammation, prevent further outbreaks, relieve itching, keep the skin supple and hydrated, and regenerate the disrupted skin barrier.
HOW TO USE
The foundation is the Bioactive Balm for Eczema (300 ml), which is applied to all affected areas. On the most resistant spots, the Bioactive Cream for Eczema (50 ml) is applied as a second layer.
With regular use, symptoms typically begin to subside after 14–21 days, with noticeable improvement after a further 3 weeks.
Even when using EPIDERMA® products, a temporary worsening may occur at the beginning (usually around one week), associated with the restoration of natural processes in the skin. This period needs to be endured and regular care must not be neglected. If pus develops, consult a dermatologist.
You can find these dermocosmetics in our online shop and at any good pharmacy.
Prevention and practical tips for every day
Although dyshidrotic eczema cannot be completely cured, proper prevention can significantly reduce the frequency and severity of flare-ups:
Identify your triggers: Keep a diary of what may precede a flare-up – contact with certain materials, foods, or stressful situations.
Avoid irritants: When working with cleaning products, solvents, or chemicals, wear protective gloves (cotton gloves under rubber ones).
Consider a low-nickel diet: If nickel allergy is confirmed, reducing nickel-rich foods may help – chocolate, legumes, nuts, shellfish, canned foods.
Limit water contact: Excessive hand washing and prolonged contact with water disrupt the skin's natural protective barrier and may worsen the condition.
Moisturise regularly: After each hand wash, apply a suitable emollient or balm.
Manage stress: Relaxation techniques, yoga, meditation, or biofeedback can help reduce the frequency of flare-ups.
Wear breathable materials: Opt for cotton gloves and socks, avoid synthetic materials.
Scientific references
1. Wollina U. Pompholyx: a review of clinical features, differential diagnosis, and management. Am J Clin Dermatol. 2010;11(5):305–14. PubMed
2. Abreu-Velez AM, Pinto FJ, Howard MS. Dyshidrotic eczema: relevance to the immune response in situ. North Am J Med Sci. 2009;1:117–120. PMC
3. Soler DC et al. The Key Role of Aquaporin 3 and Aquaporin 10 in the Pathogenesis of Pompholyx. Dermatol Ther (Heidelb). 2015;5(1):55–65. PMC
4. Yoshihisa Y, Shimizu T. Metal Allergy and Systemic Contact Dermatitis: An Overview. Dermatol Res Pract. 2012;2012:749561. PMC
5. Ahlström MG et al. Nickel allergy and allergic contact dermatitis: A clinical review. Contact Dermatitis. 2019;81(4):227–241. Wiley
6. Calle Sarmiento PM, Chango Azanza JJ. Dyshidrotic Eczema: A Common Cause of Palmar Dermatitis. Cureus. 2020;12(10):e10839. Medscape
7. Fowler JF Jr, Storrs FJ. Nickel Allergy and Dyshidrotic Eczema: Are They Related? Am J Contact Dermat. 2001;12(2):119–121. PubMed
This article is intended for informational and educational purposes only and does not replace professional medical advice. If you experience persistent symptoms, please consult a dermatologist.
|
PROFESSIONALLY REVIEWED MUDr. Jiří Skalický Founder of EPIDERMA® and author of the patented Betuldiol® composition. Graduate of Charles University in Prague (1978), specialist in inflammatory skin conditions with over 40 years of experience. |
