If this scenario sounds familiar, you may be dealing with a condition called Topical Steroid Withdrawal — the syndrome that occurs after discontinuing topical corticosteroids. TSW for short.
TSW is a topic that has literally exploded on social media in recent years. On Reddit, the r/TS_Withdrawal community has tens of thousands of members. In March 2025, a breakthrough came — researchers at the U.S. National Institutes of Health (NIH) defined diagnostic criteria for TSW for the first time and identified its biological cause as distinct from eczema. TSW is no longer just a controversy — it's becoming a recognized diagnosis.
What is Topical Steroid Withdrawal
Topical Steroid Withdrawal (TSW), sometimes called Red Skin Syndrome or corticosteroid dependency syndrome, is a rebound reaction of the skin that occurs after discontinuing topical corticosteroids. It typically affects people who have used these products for more than two to three months, often at medium to high potency, on a daily or near-daily basis.
The key thing to understand is that TSW is not the same as a return of the original eczema. It is a separate skin reaction caused specifically by the prolonged use of corticosteroids and their subsequent withdrawal. The skin develops a form of dependency — it requires ever-stronger doses for the same effect (known as tachyphylaxis) and reacts more severely after withdrawal than the original condition.
Although this phenomenon was first described in 1979, it remained controversial for a long time. Many dermatologists considered it "steroid phobia." But that's changing:
- In 2021, the UK's Medicines and Healthcare products Regulatory Agency (MHRA) officially recognized TSW as an adverse effect of corticosteroids.
- Since June 2025, information about the risk of TSW must be included on the packaging of all corticosteroid creams in the United Kingdom.
- In March 2025, an NIH team published a study that proved for the first time that TSW has a different biochemical basis than eczema — an excess of a substance called NAD+ (nicotinamide adenine dinucleotide) in the mitochondria of skin cells.
Two main types of TSW
According to the medical literature, TSW manifests in two basic forms. A person may experience symptoms of one type or a combination of both.
Erythematoedematous type
The more common and more severe variant. It presents with intense redness, swelling, oozing areas, and severe skin burning. Burning is present in up to 95% of cases of this type. The skin looks like a sunburn — hot to the touch, tight, and extremely sensitive. This type most commonly occurs in people who used corticosteroids for eczema or atopic dermatitis.
Papulopustular type
More closely resembles acne or rosacea. Red papules appear, sometimes with purulent content, on a base of reddened skin. Burning is less pronounced (around 35% of cases), but the skin is uncomfortably sensitive. This type is associated with long-term use of corticosteroids on the face.
Symptoms: How to recognize TSW
TSW symptoms can appear within hours to months after discontinuing corticosteroids. Most commonly, they begin within the first days to weeks.
- Burning and skin heat — often the very first symptom. The skin is noticeably warmer than surrounding areas (thermal dysregulation). Highly characteristic of TSW and not seen at this intensity in ordinary eczema.
- Intense redness — spreads beyond the areas where corticosteroids were applied. Confluent and diffuse, not in well-defined patches as in eczema.
- Red sleeve sign — reddened arms and forearms, but the palms remain unaffected. A specific diagnostic indicator for TSW.
- Massive peeling — the skin peels off in sheets or as a fine powder. A consequence of disrupted skin barrier.
- Intense itching — deeper and more burning than in eczema. Patients describe it as "itching from within."
- Oozing and crusting — in the acute phase, the skin may ooze and form yellowish crusts, particularly on the face and neck.
- Swelling — particularly around the eyelids and ankles. Present in approximately 43% of cases of the erythematoedematous type.
- Systemic symptoms — fatigue, trembling, chills, swollen lymph nodes, sleep disturbances, depression, and anxiety.
Important: TSW is not just a skin problem — it affects the whole person. Systemic symptoms such as fatigue, sleep disturbances, and mood changes are documented in the medical literature and are part of the clinical picture.
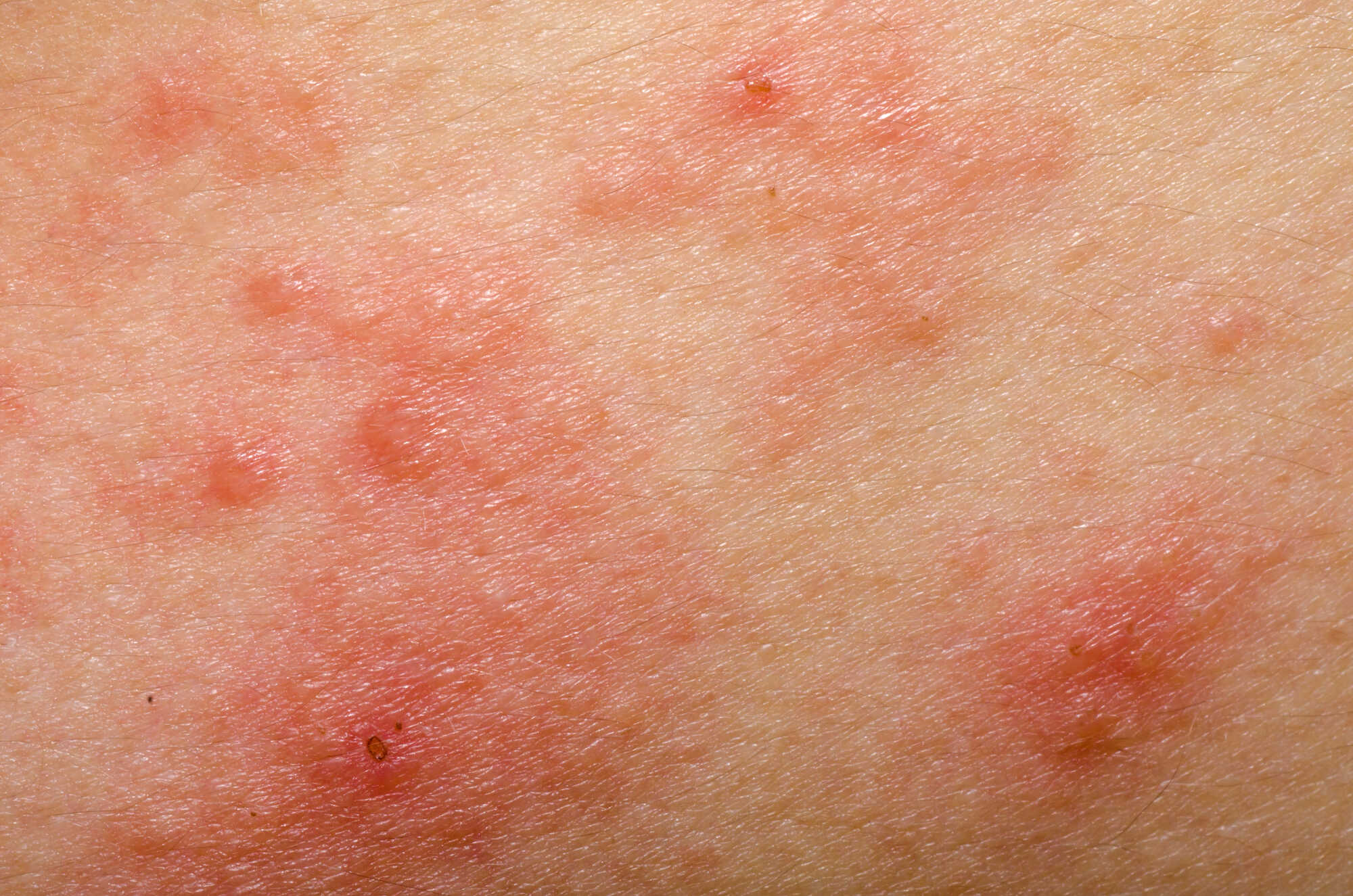
TSW versus eczema flare: How to tell them apart
This is probably the most important question. You stop corticosteroids and your skin gets worse — is it TSW, or has the eczema simply returned?
Distinguishing between them is not straightforward and should ideally be done by a dermatologist. However, there are clues. The medical literature identifies three main diagnostic criteria:
- The dominant symptom is burning, not itching. Eczema typically itches. TSW typically burns.
- Redness appears confluent and diffuse (not in well-defined patches) and develops within days to weeks after discontinuation.
- History of prolonged and frequent corticosteroid use on the affected areas, particularly the face or genital area.
The groundbreaking 2025 NIH study also identified a biochemical difference: TSW patients had elevated NAD+ levels and tryptophan metabolites (kynurenine pathway) in their skin. These changes were not present in eczema without TSW. This confirms that TSW is a distinct condition with its own mechanism.
Another practical clue is the extent of involvement. If symptoms spread to areas where you never applied corticosteroids, that's a strong argument for TSW.
What happens in the skin: The mechanism of TSW explained simply
Suppression of the skin's own cortisol production. Your skin has its own "mini adrenal glands" — keratinocytes can produce cortisol. When you supply cortisol externally over a long period, the skin shuts down its own production. After withdrawal, it's left without anti-inflammatory protection — both external and internal.
Rebound vasodilation (trampoline effect). Corticosteroids constrict blood vessels — that's why redness disappears after application. With chronic use, nitric oxide (NO) accumulates but is suppressed by the corticosteroids. After withdrawal, the accumulated NO is released all at once, vessels dilate beyond their pre-treatment state, and the result is intense redness and burning.
Skin barrier disruption. Corticosteroids thin the skin and impair the production of ceramides and other lipids that form the protective barrier. After withdrawal, the barrier is weakened, the skin loses water (increased transepidermal water loss — TEWL), is susceptible to infections, and reacts to stimuli that wouldn't have bothered it before.
NAD+ excess. The NIH study revealed that steroid withdrawal leads to overproduction of NAD+ in the mitochondria of skin cells and increased conversion of tryptophan to nicotinic acid. In a pilot study, berberine, a natural compound that blocks mitochondrial complex I, showed improvement.
Immunosuppression and microbiome. Corticosteroids suppress immunity in the skin, allowing overgrowth of Staphylococcus aureus. After withdrawal, the immune system "wakes up" and responds to this imbalance with a fierce inflammatory reaction.
Who is at risk
- Women make up the vast majority of reported cases — according to a 2025 Swedish study, 95%. This may be due to more frequent use of corticosteroids on the face and possible hormonal factors.
- Application on the face or genitals significantly increases the risk, as the skin in these areas is thinner and absorbs more of the active ingredient.
- Duration of use — most cases are associated with daily use for more than 6 months (63% of cases). However, some cases have been reported after just two weeks.
- Medium to high potency corticosteroids (Class III and IV in European classification) carry higher risk than mild formulations.
- Use without medical supervision — self-medication and repeated refills without check-ups increase the likelihood of use spiraling out of control.
Four phases of TSW progression
The course of TSW is individual, but the medical literature describes four typical phases:
- Acute eruption. Usually begins within a few days of discontinuation. The skin reddens, burns, and may ooze. Symptoms can be dramatic — often much worse than the original eczema. This phase is psychologically the most difficult.
- Dryness and itching. The skin becomes extremely dry, peels, and itches intensely. This phase can last weeks to months.
- Beginning of recovery. The skin slowly begins to heal but remains sensitive. Intermittent flares may occur — periods of improvement alternating with temporary worsening. This "wave pattern" is typical of TSW.
- Recovery. The skin gradually returns to its pre-corticosteroid state. For some people, this takes months; for others, years. Most sources report significant improvement within 6 to 12 months.
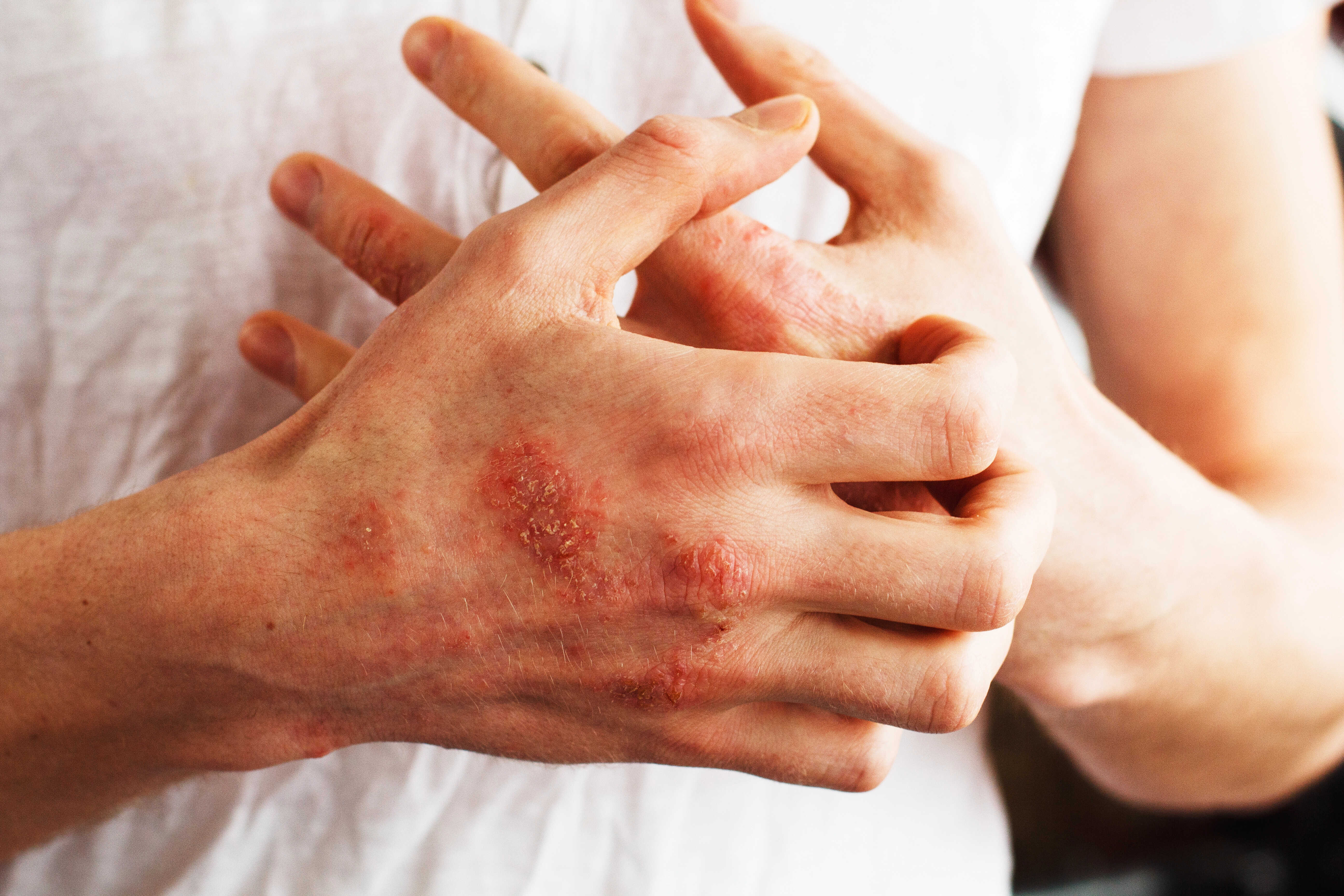
What to do if you suspect TSW
Do not stop corticosteroids abruptly on your own. Sudden discontinuation can lead to dramatic symptoms. The ideal approach is gradual tapering under medical supervision — reducing potency, then application frequency, with a gradual transition to non-steroidal care.
See a dermatologist. Ask for an examination and specifically mention TSW. If your doctor isn't familiar with the term, don't panic — it's a relatively new concept. Insist that your symptoms be taken seriously.
Get tested for contact allergy. Patch testing can reveal whether you're allergic to the corticosteroid itself or to excipients in the cream. This is more common than you might expect.
Start supportive skin care. Gentle cleansing without SLS and fragrances, light hydration, and protection of the skin barrier. Products with CBD and betulin can help reduce inflammation and support barrier repair without the risks associated with corticosteroids — which is exactly why the Epiderma range was developed with the patented Betuldiol® complex.
Take care of yourself holistically. TSW affects sleep, mental health, and overall well-being. Quality sleep, stress management, and psychological support when needed are not luxuries — they're part of the treatment.
Connect with the community. The ITSAN (International Topical Steroid Awareness Network) organization and online communities on Reddit (r/TS_Withdrawal) bring together thousands of people who have been through TSW or are currently going through it.
What the latest science says (2025)
NIH Study — Journal of Investigative Dermatology (March 2025): For the first time, it was proven that TSW has its own biochemical basis — excess mitochondrial NAD+ and activation of the kynurenine pathway. A pilot study with berberine showed symptom improvement. This opens the door to targeted treatment.
Delphi Consensus (2025): The first expert guidelines for TSW management. Recommends discontinuation of corticosteroids (both topical and systemic), dupilumab, and psychosocial support as the first line of management.
Review article in Frontiers in Allergy (March 2025): Described TSW mechanisms in detail, including the trampoline effect, Th1/Th2 imbalance, and the role of the skin microbiome.
Survey of dermatologists: 88% of British dermatologists agree that TSW needs urgent research. The era of dismissal is ending.
For patients, this means that alternative steroid-sparing approaches — including dermocosmetics with bioactive ingredients like CBD and betulin — are fully aligned with the direction the field is heading.
Frequently asked questions
Can TSW affect anyone who uses a corticosteroid cream?
Most people who use corticosteroids short-term and as directed by their doctor will not experience TSW. The risk increases with duration of use, potency of the product, and application on the face or genital area. With short-term use at low potency, the risk is very low.
How long does TSW last?
It varies — from several months to several years. The longer and at the higher potency the corticosteroids were used, the longer recovery tends to take. Most expert sources report significant improvement within 6 to 12 months.
Can TSW be treated?
No specific approved treatment currently exists. Management includes discontinuing corticosteroids (ideally gradually), supportive skin care, symptom management (cooling, antihistamines), and psychological support. In more severe cases, a dermatologist may consider dupilumab, tacrolimus, or phototherapy. The NIH berberine study showed promising results, but these are still pilot data.
Is it safe to use CBD products during TSW?
CBD has proven anti-inflammatory, anti-itch, and antimicrobial properties and is not an immunosuppressant like corticosteroids. CBD products are generally well tolerated even by sensitive skin. The Betuldiol® complex combines CBD with betulin, which supports healing and skin barrier repair. It is not a medicine for TSW, but a supportive care product that can help alleviate symptoms.
Should I stop corticosteroids all at once or gradually?
Definitely gradually, and under medical supervision. Abrupt discontinuation can lead to dramatic symptoms. Tapering — gradually reducing potency and frequency — gives the skin time to adapt. It's also important to have an alternative care strategy in place.
Can TSW affect children too?
Yes, cases in children are documented in the medical literature. Children's skin is thinner and absorbs more of the active ingredient, so particular caution is needed when prescribing corticosteroids for children.
Scientific sources
- Shobnam N, Ratley G, Saksena S et al. Topical Steroid Withdrawal is a Targetable Excess of Mitochondrial NAD+. Journal of Investigative Dermatology, 2025. doi:10.1016/j.jid.2024.11.026 · NIH Press Release
- Mohta A, Sathe NC. Topical Steroid Withdrawal (Red Skin Syndrome). StatPearls, 2024. ncbi.nlm.nih.gov/books/NBK603718
- Maskey AR, Sasaki A, Sargen M et al. Breaking the cycle: a comprehensive exploration of topical steroid addiction and withdrawal. Frontiers in Allergy, 2025; 6:1547923. doi:10.3389/falgy.2025.1547923
- Lee HK, Reiche L. Topical Corticosteroid Withdrawal. DermNet NZ, 2025. dermnetnz.org
- National Eczema Society UK. Topical Steroid Withdrawal (TSW). 2025. eczema.org
- Alsterholm M et al. Topical Steroid Withdrawal in Atopic Dermatitis: Patient-reported Characterization. Acta Dermato-Venereologica, 2025; 105. doi:10.2340/actadv.v105.40187
- Zemlok SK, Sandler M, Yu J. Initial Consensus for the Management of Topical Steroid Withdrawal: A Delphi Study. J Cutan Med Surg, 2025. doi:10.1177/17103568251388635
- Orr N et al. Reviewing the Evidence Base for TSWS. J Med Internet Res, 2024; 26:e57687. doi:10.2196/57687
This article is for educational purposes and does not replace a medical consultation. If you suspect TSW, consult your dermatologist. Epiderma products are not medicines and are not intended to treat, prevent, or diagnose diseases.
